We are always on guard when an active young teen presents with low back pain. Unlike adults who experience general low back pain, many active teens with back pain have a stress fracture in the back. We also call these injuries spondylolysis or a pars defect. How do painful pars defects of the back present, and what do we do about them?
What is the Pars Interarticularis of the Spine?
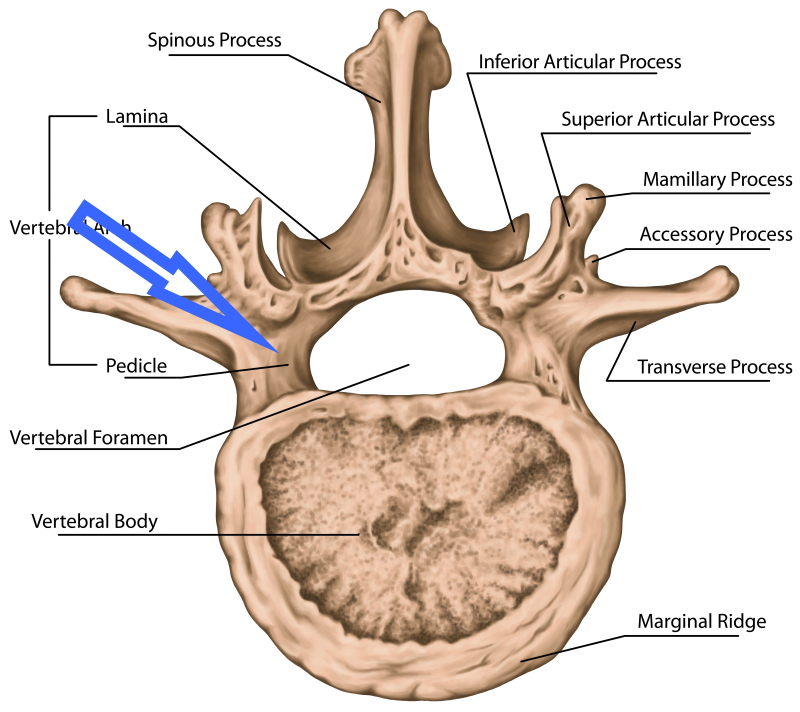
The pars interarticularis of the spine is an area at the back of each vertebra between the pedicle and lamina. This small area is more vulnerable to excessive stress because it is the last part of the vertebrae that hardens during puberty. Thus, the pars is the weakest link in the spine and the most vulnerable to bone fatigue in active teens. Pars fatigue leads to a pars defect or fracture.
Causes of a Pars Defect in the Spine.
Genetics and sporting activity are the most common risk factors for a pars defect in the back.
Firstly, some people are prone to developing a stress fracture due to the strength and shape of their bones. Generally, these factors are determined by genetics. Also, we know that you are more likely to develop a stress fracture if your sibling or parents have had one. Finally, the younger you are, the more likely you’ll have a painful pars defect. So, an active 10-year-old is more likely to have a painful pars defect than a 19-year-old.
Secondly, repeated extension and rotation sports can lead to bone fatigue. These sports include gymnastics, tennis, cricket, bowling, swimming, and diving. However, competitive runners can also develop stress fractures.
What are the Most Common Findings of a Painful Pars Defect in the Back?
Generally, active teens report low back pain that doesn’t settle with a short rest period (2-4 weeks). Pain is usually worse with sports like swimming, diving, athletics, tennis, cricket, and bowling. This is because the athlete experiences pain when the spine is rotated. Often, the pain settles quickly with rest and flares again with sport.
Teenagers are tender in the lower back. However, a study by Dr Masci showed that examination was not a good indicator of whether a patient had a painful pars defect.
Sometimes, if fractures occur on both sides of a vertebra, the spine can slip, causing spondylolisthesis. If a significant slip occurs, the teen reports pain going down the leg. Occasionally, numbness, pins and needles, or muscle weakness occur. However, most slips are small, and large slips are very rare.
How Do We Diagnose a Painful Pars Defect in the Back?

Generally, an X-ray is not a good test as it can miss many pars fractures.
Traditionally, we used bone scans to detect high bone activity. MRI has recently become the test of choice as it is quick, easy, and does not expose the teen to radiation. Dr Masci found in his study that MRIs missed a few painful pars defects compared to bone scans. Recently, new technology and more powerful scanners have made MRI more sensitive to detecting bone stress. However, it is still essential to use specialised MRI pictures to increase the pick-up rate.
We use MRI and CT scans to detect fractures. However, CT scans expose young athletes to radiation, which we want to avoid. Recently, a specialised MRI called VIBE has been shown to detect fractures better than traditional MRI and is now replacing CT scans.
So, if you are concerned about a stress fracture in the back, you should have a specialised MRI scan with specific VIBE sequences to increase the pick-up rate.
What is the Treatment for a Painful Pars Defect in the Back?
In general, most active teens with an acute pars fracture will settle with a period of rehab and rest from the sport.
Overall, the time out of sport depends on how early the pars fracture is detected. Early detection means the young athlete may only need to rest for a few weeks. Also, early detection means that a bone break—a term known as a fracture—is less likely. Nonetheless, the development of a fracture does not mean a worse outcome.
Most athletes undertake supervised rehab to improve spine mobility. Time out of sport will depend on pain severity and the presence of a fracture. Depending on pain levels, we suggest a slow and progressive return to training and sport.
Often, we repeat MRI scans with VIBE sequences to check for bony healing. Athletes should not return to high-load activities and sports until scans show evidence of reduced bone swelling +/- healed fractures. However, sometimes fractures don’t heal, so returning to sports will be based on improvement in pain and function.
Should we brace a painful pars defect?
Generally, we discourage bracing as it does not improve healing. A recent study suggested that bracing does not improve fracture healing or accelerate return to sport. Also, bracing leads to significant deconditioning, which may increase the risk of a repeat stress fracture at the same or a different site. We also know that repeat stress fractures take longer to heal.
Bracing is occasionally used for younger patients with severe pain who can’t sit still and require enforced rest. Even then, a brace is only used to relieve pain and is needed for only a short time (6 weeks).
Surgery should only be considered for a few cases of stress fracture that fail to settle or develop a significant slip known as Spondylolisthesis. Most slips are mild and don’t progress into larger slips. Generally, surgery for pars stress fractures has a long recovery, and some athletes don’t return to their sport after surgery.
Other Common Questions about a Pars Defect in the Back.
Is a pars stress fracture the only cause of low back pain in active teens?
Other factors, such as a disc injury or muscle tear, can cause low back pain. Usually, these injuries settle relatively quickly with rest from sport. However, assessing the back for bone stress is essential if the pain does not resolve with a short rest period.
Is bracing needed for a pars stress fracture?
We think not. Bracing has not been shown to improve healing compared to rest from sport. We only use a brace to settle pain in younger athletes and keep them still.
Is lumbar Spondylolysis serious?
Lumbar spondylolysis is another name for a pars defect or a pars stress fracture. Generally, lumbar Spondylolysis will settle with rest from activity and physiotherapy. Early diagnosis is critical for managing lumbar Spondylolysis, leading to less time out of sport.
Spondylolysis vs Spondylolisthesis: What is the difference?
Spondylolysis refers to pars defects. Spondylolisthesis is a slip of the spine that occurs after bilateral spondylolysis or a pars defect at one level. Generally, Spondylolisthesis is rare but can occur in younger teenagers during puberty. Sometimes, these slips can progress, leading to nerve pinching and leg pain. However, after puberty, it is unlikely the slip will worsen.
Most slips are mild and don’t need surgery. Also, having a slip does not exclude teenagers from sports, including contact sports.
Are Pars defects in adults painful?
Not usually. Pars defects are a common finding in about 10% of adults. Rarely are pars defects the cause of low back pain in adults. Often, back pain is due to other pathologies, such as disc or facet joint degeneration. Also, a pars defect does not necessarily mean people are more prone to back pain.
Does an MRI scan pick up all cases of active pars stress fractures?
No. In a 2004 study, we found that MRI missed about 20% of cases. So, a normal MRI scan doesn’t necessarily exclude a stress fracture. In these cases where suspicion is high but the MRI scan is normal, Dr Masci uses a more sensitive SPECT/CT scan.
Final word from Sportdoctorlondon about Spondylolysis
Stress fractures in the back are common and often cause low back pain in active teens. Early MRI detection is vital to reduce time out of sport. Finally, most cases will settle with rehab, spine mobility and strengthening. Surgery is discouraged and rarely required.


I hope you are well.
I am reaching out regarding my 15-year-old daughter, Kailah Pickston, who has been struggling with ongoing spinal issues, including a bilateral pars defect and moderate scoliosis (17 degrees).
Medical Background:
• Two years ago, Kailah was diagnosed with a bilateral pars defect and was placed in a hip spica cast for four months. The left side appeared to heal, but no CT scan was performed at the time to confirm whether the right side had fully healed. Kailah was then discharged and advised to resume normal activities.
• In May/June last year, I sought private physiotherapy for her, and she gradually returned to netball in September. However, by January, her pain had returned and worsened.
• A recent CT scan has now revealed a new fracture on the left side, along with incomplete healing on the right.
• She also has moderate scoliosis (17 degrees), which may be affecting her biomechanics and contributing to her ongoing discomfort.
• Current condition: Kailah is no longer participating in netball or any other sports. She experiences constant pain, particularly when sitting, standing, being bumped, or even sneezing. Last week, her pain escalated from a 6 to a 9, leading me to take her to urgent care, where she was prescribed codeine.
• This once active and enthusiastic athlete is now afraid to move. Her walk shows clear signs of self-protection, and this is having a significant impact on both her physical and mental health.
Concerns with Current Care at RNOH:
• Kailah is currently under the care of the Royal National Orthopaedic Hospital (RNOH), but we have concerns that their approach does not fully take into account the cause of the new fracture on the left side or how the ongoing issues on the right may be affecting it.
• Their current advice is simply to stop movement, allow the left side to heal again, and repeat this process, which has not been effective so far.
• The consultants at RNOH have been very negative about surgical options and do not seem familiar with minimally invasive pars repair procedures.
Seeking Your Expertise:
We are exploring alternative treatment options and would like to know whether you may be able to help,
I would greatly appreciate the opportunity to discuss this further, either in person or via a virtual consultation. Please let me know if you would be available, and what the next steps would be to arrange an appointment.
Thank you for your time, and I look forward to your response.
Kind regards,
Jenny Pickston
07476716923
Many thanks for your query. I have responded to you by email.
Lorenzo
My daughter was assessed for suspected pars defect. After 6 weeks of total rest from sharp pain onset disappeared, but lately some pain is back. However both X-ray and MRI are negative for pars defect. Would you recommend a CT scan?
In cases where I suspect a pars defect but MRI is normal, I consider a SPECT/CT scan (which is a combination of a bone scan and CT scan). i performed a study over 20 years ago comparing SPECT/CT with MRI in pars defects and found that MRI misses about 20% of cases.
Lorenzo
Hi Dr. Masci, My 17-y-o son had an MRI-confirmed lower-lumbar stress fracture in August 2025. He had been experiencing pain while pitching (baseball) for much of the summer and the prior spring but did not have pain hitting or playing other positions, or doing other activities. He underwent active physical therapy throughout the fall and returned to training for baseball pain-free in December.
He was pitching in a game yesterday and felt the same pain he had last year, and immediately took himself out of the game. We’re going back to his orthopedic this week and of course will seek another MRI to assess.
My question: This kid LIVES for baseball and the high school season runs another month. Can he conceivably play the rest of this season IF he’s pain free (i.e. doesn’t pitch), perhaps while wearing some kind of wrap around his lower torso and then take a couple months of summer to follow the rest/PT protocol? Or would that be too risky in terms of possible progression of the injury to something far more serious?
Obviously not asking you to Dx a patient over the Internet, nor am I committing him to any specific action based on your opinion but just want to get a perspective, with the awareness that he clearly played for 3+ months with this injury last year before we had it diagnosed.
Thanks in advance for any input at all.
Best,
John
Dear John,
Thank you for such a thoughtful and well-considered message.
A few important points in response:
First, I would not automatically presume that your son’s recurrent pain is due to pars stress at the same level. It may not be — which is exactly why the MRI is pivotal before drawing any conclusions or making decisions about return to play. The scan will tell us what we are actually dealing with.
Regarding playing through the season: this really does depend on what the MRI shows. That said, I want to be clear about my general philosophy — I tend to feel that we should be more aggressive with the management of pars bone stress injuries, not less. Early offloading leads to better outcomes and a quicker return to play in the long run. The temptation to play through it is understandable, but the risk is prolonging the overall recovery significantly.
There is also something worth knowing: studies show that recurrent stress fractures occurring in the same location as a previous injury tend to take longer to heal. This may be related to reduced local bone density as a consequence of the previous injury and the rest period that followed. This is another reason not to underestimate a recurrence.
Ultimately, I would strongly encourage you to be guided by your son’s orthopaedic surgeon or sports medicine doctor, who will be able to review the MRI findings in full and give you specific, individualised advice.
I hope that gives you a useful perspective. Good luck to him.
LM